This blog post may contain affiliate links. I earn a small commission on your purchase, at no cost to you.
When I got my MS diagnosis in October 2025, I realized pretty quickly that I didn't actually know what MS was. I knew the name. I'd heard it. But knowing the name of something and understanding what it's doing inside your body are two completely different conversations.
So I did what I do. I researched. I read. I asked questions. And then I thought about all the women who might be sitting where I was sitting — newly diagnosed, overwhelmed, and Googling at midnight — and decided to write the post I wish someone had handed me.
This is that post.
Okay, But What Actually Is MS?
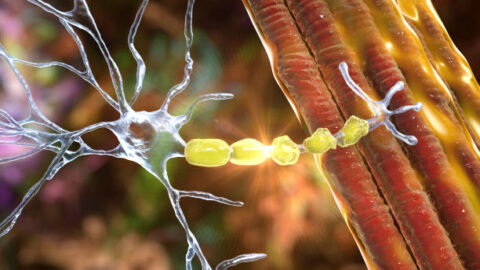
Multiple Sclerosis is an autoimmune disease, which means your immune system, the very thing that's supposed to protect you, gets confused and attacks your own body instead. Specifically, it attacks the myelin sheath, the protective coating around your nerve fibers. Think of myelin like the rubber insulation around an electrical cord. When that insulation is damaged, the signals traveling through the wire get scrambled, slowed, or stopped altogether.
Those scrambled signals? That's your symptoms.
The damage shows up as lesions, areas of scar tissue on the brain and spinal cord. The word "sclerosis" literally means "scarring," and "multiple" refers to the fact that these lesions appear in more than one place. Your nervous system is just out here getting attacked from several directions at once.
There is currently no cure. But, and this matters, there are more treatment options now than ever before, and people are living full, meaningful lives with MS. This tidbit is what has kept me from spiraling.
What Does MS Feel Like? Common Symptoms
Here's the thing that tripped me up for years: MS symptoms are wildly nonspecific. They overlap with grief. With perimenopause. Being a Black woman in her 40s, who is tired because she is doing a lot. Here's what the symptom list actually looks like:
- Fatigue — not regular tired, but a bone-deep exhaustion that doesn't respond to sleep the way you'd expect
- Numbness or tingling — in the face, arms, legs, or body, sometimes coming and going
- Brain fog / cognitive issues — difficulty concentrating, memory lapses, trouble finding words
- Vision problems — blurred vision, double vision, or pain when moving the eyes (optic neuritis is often one of the first signs)
- Muscle weakness or spasticity — stiffness, spasms, difficulty with coordination or balance
- Heat sensitivity — symptoms that get noticeably worse when your body temperature rises (this one is called Uhthoff's phenomenon, and it is very real)
- Bladder and bowel issues — urgency, frequency, difficulty fully emptying
- Mood changes — depression and anxiety are common with MS, and not just as a reaction to the diagnosis
Some of these symptoms come and go. Some stick around. Some you won't have at all. That's the other thing about MS: it is deeply personal in how it shows up, which is part of what makes it so difficult to catch.
The Different Types of MS
Not all MS is the same. There are four recognized types:
- Relapsing-Remitting MS (RRMS) — the most common type, affecting about 85% of people at diagnosis. You have flares (relapses) where symptoms worsen, followed by periods of partial or full recovery (remission). This is my diagnosis.
- Secondary Progressive MS (SPMS) — many people who start with RRMS eventually transition to this type, where the disease begins to steadily progress with or without clear relapses.
- Primary Progressive MS (PPMS) — about 15% of people are diagnosed with this type from the start. There are no distinct relapses — instead, neurological function gradually declines from the beginning.
- Progressive Relapsing MS (PRMS) — the rarest form. Steady progression from the start, but with clear relapses along the way.
Your type matters because it shapes your treatment options and what you can expect. If you're newly diagnosed, ask your neurologist specifically which type you have and why.
Who Gets MS?
For a long time, the medical community treated MS like it was a white woman's disease. European ancestry. Northern climates. Young adults between 20 and 40. That framing has done real harm, because it meant a lot of people — especially Black women — weren't being looked for when they walked into a doctor's office with symptoms.
Here's what the research actually shows:
And bear with me as I remember how to cite sources properly.
According to Washington University Arts & Sciences, Black women have roughly a 60% higher risk of developing MS compared to white women. Not lower. Higher. And yet MS has traditionally been thought of as a young white woman's disease, which means doctors may not consider MS when a Black patient presents with certain symptoms. (HealthyWomen)
Many African American women have reported that their MS diagnosis was a surprise to both them and their doctors, and that their diagnosis had been delayed while physicians initially focused on other conditions considered more typical in Black patients. (PubMed Central)
Think about that. The disease is more common in us, and we're still the last ones to get diagnosed. Figures.
Black people with MS may be older at the time of diagnosis, experience more severe symptoms, and have faster disease progression. (Genentech) Part of that is almost certainly because, by the time many of us get the diagnosis, the disease has had years to do its unchecked work.
Someone complaining of numbness in the arm might be told it's a pinched nerve. My original diagnosis. Fatigue gets written off as stress. Because MS symptoms can go away and not return for a while, a person might think what they experienced was just a passing issue (which I did) and not seek further treatment until it returns. HealthyWomen
Sound familiar? It should. I lived that story for six years.
Women overall are diagnosed at three times the rate of men. MS also tends to run in families, though not in a simple parent-to-child way; it might show up in a cousin, an aunt, or a grandparent.
How Is MS Diagnosed?
There is no single test that definitively says "you have MS." Diagnosis involves a combination of your symptoms and history, an MRI of the brain and spinal cord (looking for lesions), a neurological exam, and sometimes a spinal fluid analysis. The diagnostic criteria were actually updated in 2024, which means MS can now be diagnosed in people with nonspecific symptom presentations, such as isolated headaches, fatigue, and nonspecific neurological issues, that previously made it much harder to get a clear diagnosis. PubMed Central
That's meaningful. That's the kind of update that might have found me sooner.
If you are pushing for answers and not getting them, ask specifically about an MRI and a neurology referral. Be persistent. Write down your symptoms and when they happen. Bring someone with you if you can. The system isn't set up to make this easy for us, so we have to make it harder to dismiss.
One More Thing
If you are a Black woman and something has been feeling off — fatigue that won't lift, numbness that comes and goes, vision weirdness, brain fog that doesn't match your stress level — please don't do what I did. Don't spend six years explaining it away.
You know your body. Trust what it's telling you, even when the people around you aren't listening yet.
Want to read my full diagnosis story? That post is >here<.
Want to see what’s in my actual day-to-day care kit? That post is >here<.